Tag: ACA
ACA Then, Now, and Tomorrow. Measuring Success or Failure.
New Web Site. New effort. Old news updated. The ACA then and now.
I was looking at my archives and found Notes & Links: October 21, 2013. I posted a piece that Dan Munro a healthcare contributor at Fobes had on Obamacare Numbers Success or Failure? Munro noted that there were 476,000 health insurance application were filled through ACA Federal and State exchanges. Since then we can say a few more Americans have applied with over 20 million people have health insurance either through public o private options. As of December 24, 2016 there were 11.5 million people who used the federal marketplace to buy health insurance. 8.9 million renewed their coverage or bought new plans to replace existing plans. 2.6 million new people enrolled. It was so cute that Munro ends that piece from 2013 noting that the ACA is the single biggest target on Obama’s back. You think.
Fast forward to Munro article in Forbes Trump Acknowledges That The ‘Replacement’ Of Obamacare Will Span Years. This was pulled from President Trumps interview with Bill O’Reilly. Besides the fact Trump is seeing that the ACA can’t be just turned off without doing great harm to millions of Americans. Ultimately in rich and ironic way the GOP is being forced think about outcomes that are not tied to punishing former President Obama. GOP oh my. Which brings me to my final thought here.
As the ACA is repealed, replaced, or repaired there will be reams of pages written about the harm these actions will have on the sick, the old, and the young. There will be competing projections of what these changes will produce. For now the little we know about what will be done or considered is not enough to get our outcomes arms around.
I would like to imagine that someone, some academic institution, some group of thinkers will set up a site to track key healthcare outcomes retrospectively from the beginning of the ACA to its ‘repair’ and then going forward. Surely there will be measures of those who have and don’t have health insurance and measures of cost of health insurance and more. I am hoping we can get into the granular data that may takes years to revel a trend.
Just to throw out some ideas: Measure standards of care treatments and their outcomes for specific conditions. Compare Repaired ACA to Pre-Repaired to Non-ACA health insurance. Will we see worse outcomes in one group vs. the other group?. Are treatments offered as first line differ between measured segments? Is the life expectancy for similar diseases and patients shorter or longer between segments?
I am not a statistician nor an epidemiologist (obviously). So I’m not sure any of this can be done. Should it be done? Yes, because this is the type of evidence (not alternative facts) that the fix and repair GOP made into law. We need to know if it’s keeping Americans alive and healthy. This GOP driven destruction of Americas health is similar to the Death Panels feared in 2012 by the GOP. Now they get to enact their dream, thinning the herd of poor, sick, and non-GOP voters.
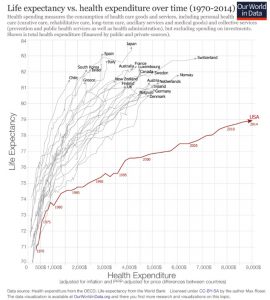
Bonus link, One World In Data. Really great charts and graphs on healthcare.
Speaking of Media Morons: Fox, ACA, and Reality
Aaron Carroll at The Incidental Economist responded to a Fox news story about a family that could not find a healthcare policy for their 1 1/2 year old. And of course they are blaming Obamacare since it was on Fox, no surprise there.
I have turned a deaf ear to these stories and that source in particular. But Carroll took aim and deconstructed it to the point of discrediting the spot so well. Hop to the site and read his five points. The Fox news report seriously shows to what degree the loyal opposition will go to make sure people will not sign up, hate the President, and avoid insurance.
Carroll makes a great point that does a Jon Stewart showing the hypocracy.
I’m sorry, but I find it somewhat hypocritical that only now, after decades of about 50 million people being uninsured every year, that suddenly the media is outraged by stories of people (healthy, mind you) having difficulties finding insurance. Really? Suddenly this is an issue? Didn’t seem like it before… AND THIS STORY IS ALREADY RESOLVED. AND LIKELY NOT ENTIRELY TRUE.
Notes & Links: November 15, 2013
Stefan Larsson: What doctors can learn from each other
An important TED talk about creating patient value in healthcare through outcomes that matter. At the center of this talk is the very simple idea of when physicians share with each other their clinical work (i.e.say hip replacement) and through that sharing create a list of outcomes that patients value those physicians improve outcomes and lower costs. Larsson identifies this as continuous improvement since this process of meeting, sharing, and ranking physicians work happens annually. What occurs is that those physician who may be at the bottom half change behavior and move up. New techniques are introduced and those who may have moved down on measured outcomes can now move up.
What strikes me hearing this talk is that it mimics constructivism which simply stated is the process of integrating new knowledge with existing knowledge to create new. That is what is occurring here is discovery, it is linking new information to prior knowledge and helping physicians improve care.
Most TED videos are brilliant but this one touches on so much we are doing and talking about regarding healthcare.
Obamacare And The End Of Employer-Based Health Insurance
Peter Ubel contributing to Forbes does and excellent job of clearing the underbrush in our current employee based healthcare system. Next he tackles Analysis & Commentary from Health Affairs “Will Emplyers Drop Health Insurance Coverage Because of the Affordable Care Act? written by Thomas Buchmueller et. al. out of University of Michigan. What is interesting in this analysis by Ubel is that he demonstrates why large companies can afford to keep giving health insurance and small ones don’t.
Because of their large size, these companies are able to negotiate lower premiums with insurance companies, because they have enough employees to reduce their actuarial risks. If a company employing 10 people is unlucky enough for one of their employees to experience a serious cancer diagnosis, for example, the insurance company offering coverage for this company will lose money on that company’s business. By contrast, there is not much chance that a company with 5000 employees will have 500 of their employees develop cancer over the next year. Big numbers reduce risk. And reduced risk means lower insurance premiums.
So on my reading large companies are behaving in classic free market economics. They can afford to offer insurance since there is a pooled risk. Small companies can’t. Therefore small companies can’t compete.
Offering healthcare to all and trying to make it affordable we are improving competition. Though the cost, which Ubel presents in the next few paragraphs works against the small company due to wages paid. On some level we need to consider ACA as a tool to help not just people live longer and better, we need to think of it as a way for small companies to compete for talent with the large companies.
Performance measurement and the new cholesterol guidelines
Rcentor at db’s Medical Rants takes a moment of clarify the new cholesterol guidelines and put them into perspective.
The new cholesterol guidelines have responded to a series of studies and analyses that have made clear that lowering the cholesterol is not the magic goal, rather statins (which clearly lower cholesterol) are “magic” but probably because of their pleiotropic effects.
The primary consideration here is that doing performance measurements based on guidelines may miss the point and it takes time to correct course. Once you’ve read the new guidelines take a look at this for its measured thoughts on why these new guidelines are important.
What Closed Circuit TV Can Tell Retailers About Customers
Streetfight interviews Steve Russell the founder of Prism Skylabs that is a startup in Sand Francisco who offers retailers software to analyzes video streams looking at traffic, heat maps, etc. It is interesting that those CC videos used to catch shoplifters at Barney’s, Wrongly. Can not be used to analyze customers behavior.
It’s a shame that we can’t use this to measure the behavior of patients on learning about their health and what they do with data. It can be done but not as easily as watching a video tape.
The Myth of Patient-Centered Care
Steve Wilkins posting at Healthworks Collective makes a cogent and important argument and solution to
Findings from BJM Quality and Safety article, and other like it, suggest that health care providers today are no more patient-centered in the way they communicate with patients than they were 30 years ago when research into the dynamics of physician-patient communication first began.
Even though physicians failure to inquire about patients expectation is not about understanding how important it is. It was lack of communications skills and know how. They do what they did 30 years ago which is not much.
But Wilkins jumps into the fray with a solution
Helping raise awareness of the state of physician-patient communications in the U.S. is why I have taken the lead in bringing together some of the leading authorities in the physician-patient communication filed to organize the Adopt One! Challenge. Adopt One! challenges physicians across the country to take the first step by committing to adopt one new patient-centered communication skill in 2014.
It is nice to see people looking at strategic solutions based on data.
America’s cancer care crisis-is Europe any better?
Lawler, Duffy, La Vecchia, et. al. writing in The Lancet points out that America’s cancer care crisis and how optimum health care and raising costs are driving inequalities in treatments and outcomes. The authors examining the International Cancer Benchmarking Partnership (ICBP) that those issues demonstrated in America exist in Australia, Canada, and Sweden. And cancer mortality remains higher in central and eastern Europe than the rest of the continent, largely due to delayed diagnosis or access to treatment.
Another issue common to the IOM and ICBP reports is inequality in treatment of elderly people with cancer. Ageism in intention to treat could have profound negative effects on cancer outcomes, particularly in view of recent projections of population ageing. Unless our philosophy for treating older patients changes fundamentally, the welcome increase in cancer survivors that we are currently experiencing will be reversed.
Hard to consider that any gains we’ve made in cancer diagnosis and treatment may reverse. Well I guess we can say here is one statistic where we on par with other developed countries.
Notes & Links: November 13, 2013
The Complex Relationship of Realspace Events and Messages in Cyberspace: Case Study of Influenza and Pertussis Using Tweets
Nagel, Tsou, Spitzberg, et. al publishing an original paper in JMIR examine the internet and real time surveillance. The authors focused on Twitter. They wanted to explore the interaction between cyberspace message activity specific to Tweets and real world occurrence of influenza and pertussis.
In general, correlation coefficients were stronger in the flu analysis compared to the pertussis analysis. Within each analysis, flu tweets were more strongly correlated with ILI rates than influenza tweets, and whooping cough tweets correlated more strongly with pertussis incidence than pertussis tweets. Nonretweets correlated more with disease occurrence than retweets, and tweets without a URL Web address correlated better with actual incidence than those with a URL Web address primarily for the flu tweets.
The authors concluded that keyword choice is critical in how well tweets correlate with disease occurrence. Makes sense.
Dead Man Walking
NEJM has perspective from Stillman and Tailor that speaks to the real reasons we need healthcare in the country and why the screaming voices wanting to shutdown the ACA or pointing out the problems with the web sites are missing the reality, we as a nation needs to care for and serve Americans, all Americans not just the ones who are lucky enough to have health insurance.
Public Reporting, Consumerism, and Patient Empowerment
Huckman and Kelley writing in the NEJM offer insight and hope for what we are seeing in the press and online. Perhaps, just perhaps we are at a tipping point in our American healthcare mess. Patients are becoming healthcare consumers and are beaming more and more empowered based on reporting by healthcare providers.
Consider this, healthcare providers are reporting cost and quality metrics. What the authors contend may be needed is data needs to help patients determine is the treatment/procedure the option for my need, budget, and personal and family situation?
The rub here is that who is going to explain this to the patients/consumers? HCP are not getting paid for cognitive services. And there is a cost associated with developing and sharing this information. And will they hire old marketing communications pro’s like me to do this so they can deliver care?
6 Lies We Tell Ourselves
No, two of them are not those. Digital Tonto makes us stop and take a hard look at our business strategy acumen. Here are the six. Hope over to see the details.
1. I’m Rational And Make Decisions Based On Facts
In reality, we rarely have the time or inclination to think things through, so we take shortcuts called cognitive biases.
2. I’m Above Average
Research in a variety of has consistently shown that when people are asked to rate themselves on just about anything—their professional skill, driving ability, honesty— a majority believes that they are better than most.
3. My Competition Will be Static As I Transform
“The same fundamental error is also common in business life. Strategy sessions are big on charts and graphs, but you rarely see any scenario planning.”
4. My Employees Love (And I Inspire Them)
“The truth is that power relationships are inherently mistrustful because one side can more easily opt out. People who work for us have a strong incentive to make us believe they like us a whole lot more than they actually do, but research has shown that employees opinions are rarely aligned with their superiors.”
5. I Have The Right Information
“We’re wired to jump to conclusions if our evidence is consistent, even if is incomplete.”
6. It’s Not My Fault And I Deserve All the Credit
“When things go well we feel a justifiable sense of pride. We worked hard, we worked smart and we prevailed. We believe that we should be rewarded and are angry if we are not. On the other hand, when things don’t go our way, there are always mitigating circumstances and we don’t think we should be penalized.”
Greg does his usual excellent job at making us all stop and see the reality not the unicorn rainbows.
Quote: Uwe (Need I say More?)
Austin Frakt has a quoted from Uwe Reinhardt in JAMA. I will take the liberty of copying it here since it is some important that I would hate to see you not jump to it.
[T]he often advanced idea that American patients should have “more skin in the game” through higher cost sharing, inducing them to shop around for cost-effective health care, so far has been about as sensible as blindfolding shoppers entering a department store in the hope that inside they can and will then shop smartly for the merchandise they seek. So far the application of this idea in practice has been as silly as it has been cruel. […]
In their almost united opposition to government, US physicians and health care organizations have always paid lip service to the virtue of market, possibly without fully understanding what market actually means outside a safe fortress that keeps prices and quality of services opaque from potential buyers. Reference pricing for health care coupled with full transparency of those prices is one manifestation of raw market forces at work.
Why Local Marketers Need to Start Thinking About Their Instagram Strategy
Okay I confess I have been a long time fun maker of Instagram calling it Twitter for people who can’t read. ( I am hearing the G and T of GTFH reminding me that good marketing and communications that captures attention uses graphics with copy). Street Fight makes a great argument on why we, no I, need to consider it.
More than anything, Instagram presents an unparalleled opportunity to build and share a brand — to show a different side by leveraging this highly visual medium. Plus, the rate of customer engagement is off the charts compared to other social channels
Great read but I would guess most of you are already heavy users of Instagram. If not see why and what a local business, healthcare provider, physician practice, etc. should consider it part of a social media strategy.
Video Break for the Day
GoPro: Combing Valparaiso’s Hills
Just watch it. Makes you want to be a 20 something again this time sans the 60s drama.
Notes & Links: November 1, 2013
IMS: Half of Android health apps have fewer than 500 downloads
The report by IMS ends with the following:
The report also identifies a number of barriers that need to be addressed to increase app adoption and improve the quality of apps, including a curation platform of some kind, app integration with other parts of care, better safety and security, and more robust efficacy measures to prove the value of apps to all stakeholders in the ecosystem.
Pair that with the following from the same report and what we have is, let’s throw some poop against the wall and see what sticks. I am not sure that any consideration of strategies, objectives, etc. are made when launching these apps. And it is not as if there is not seasoned smart healthcare executives available to help. Oh wait we are old and can’t code. Gee look how well you’re doing.
Analysis of the widely available consumer healthcare apps on the iTunes app store shows that at present there are 159 apps which link to sensors,” IMS writes in the report. “However these are dominated by fitness and weight apps which monitor pulse rates when exercising and measure weight and body mass index (BMI). Fewer than 50 of these 159 apps relate to actual condition management or provide tools and calculators for users to measure their vitals. There is therefore considerable room for growth in this sector.
Sociotechnical Challenges and Progress in Using Social Media for Health
Munson, Cavusoglu, Frish, et. al out of the University of Washington shared their view on social media in healthcare and how these tools that hold so much promise are not meeting their established goals. This is a long well referenced piece that has many nuggets of knowledge. I must say it is hard to read. Damn near turgid. Of course it may be my modest IQ but I shared the work with colleagues and they felt the same.
At a recent Peter Wall Institute for Advanced Studies workshop, our group was tasked with reflecting on contemporary and coming technical challenges for using social media to promote healthy behaviors, communicate health information, and to gather information on current health behaviors or events. We hope to see a continuation and extension of recent technical developments in sensing, connectivity, and large-scale data aggregation and analysis. There are clear areas for improvement—for example, activity inference can be unreliable and drains battery life, and Google Flu is still poor at detecting atypical flu trends, as the most severe often are. We believe, however, that these challenges are being fairly well addressed by current research and market forces, and thus we do not dwell on them here.
Grab a coffee, print this out, and explore all it has to offer. The next step will be assigning sets of goals and strategies to what is presented here in clear simple language.
An Epidemic Out of Control: Poor Children and Psychiatric Drugs
Howard Brody, MD, PhD writing on Hooked: Ethics, Medicine, and Pharma reports from the American Society for Bioethics and Humanities a presentation by Dr. Melody J. Slashinski of the Center for Medical Ethics and Health Policy at Baylor College of Medicine.
Slashinski’s presentation was based on discussion with mothers and their ‘folk-knowledge network’ linking them and information about drugs commonly prescribed for children today.
That might sound easy to do, but the data went on to show that it’s extremely difficult in this population especially. The mothers also feared, quite realistically, that any evidence of “medical noncompliance” on their part would end up with a report to Protective Services and eventually losing custody of their children. So the stories Dr. Slashinski told generally depicted a delicate balancing act—moms on the one hand certain that they would not give these medicines to their children, and on the other hand going through as many hoops as they could to appearcompliant and submissive to the medical system so as not to set off alarms.
There is a long passage where Dr. Slashinski speaks to a pediatrician’s office check-up for a 9 year-old son and 8-year old daughter she witnessed. You must read the entire description but here is part of it.
The doctor then examined the daughter and said something at one point about her “boobies.” The daughter apparently became offended by this comment and stopped cooperating with the exam. The doctor immediately asked the mother how often the daughter had these “tantrums” and started talking about the possibility of bipolar disorder.
Brody’s post and his comments speaks to the massive level of drugs that are being prescribed to poor children and to the reality that parents of these children find the only way parents can protect them is by not taking them to the physician.
Can Everybody Please Just Calm Down?
Ann Mond Johnson writing on the Healthcare Blog gives another perspective on Obamacare and the whirling Dervishes surrounding its failed launch. Johnson asks that the private sector to step up to the plate and “counteract what much of the media refers to as a complete debacle”.
- First, just calm down and focus on helping clear up the confusion
- Help people shop remind people of their options under this healthcare plan
- Provide perspective Americans must have healthcare by law and now that is easier
There are voices out there who are rational, not shrill, that speak to the need for the ACA to be successful for the health of America. We all should try and find these voices and listen if for no other reason but to calm the !*#@ down.
What Would Darwin Think Of Obama’s Health Insurance Exchanges?
Ian Shepherdson a contributor at Forbes gives us another step away from that epic disaster of a launch called Obamacare and its Insurance Exchanges breach birth.
Amid the chaos, it is easy to overlook the key point, which is that the insurance exchanges are here to stay. Despite their difficult birth, they will evolve over time as lessons are learned, bad technology is fixed, and operational difficulties are overcome. They will persist, even if a future Republican administration succeeds in unravelling some elements of Obamacare.
Shepherdson goes on to point to the fact the idea which was originally a Republican concept in the 80’s. But the primary message is this is not easy task making a sea change to a nations healthcare and a change that hopefully will manage costs and improve outcomes. Those are huge targets sitting on the back of anyone trying to make Obamacare work.
Good ideas spread, unless something really powerful gets in their way. Next time you swat away a mosquito, remember how it got to be buzzing around your ear in the first place. Insects were the first flying creatures on earth, but they didn’t always have wings. They didn’t really fly, either. Instead, a random mutation in the genetic code of a non-flying insect affected the shape of its body, helping it hop or jump a bit further than its siblings, or ensuring it was blown a bit further by the wind.
Another rational voice. Perhaps I am looking for hope for America’s healthcare crisis.
Notes & Links: October 29, 2013
Making Health Addictive
Joseph Kvedar writing on HealthWorks Collective is presents the premiss that people’s addictive relationship with their smartphone can be leveraged to improve health. Kvedar admits right up front “…is there any way health can really be addictive? Probably not.” What he wants to present is the “juxtaposition of motivational health messaging with some other additive behavior, specifically checking your smartphone.”
Next comes the science of checking our phones 100 times a day (I’ll raise my hand) and how that is addictive and it releases dopamine associated with ingestion of addictive substances. Yup we get off on our phones looking for emails, stock news, weather reports, news, cat videos, etc. So far still good.
Why are smartphones so additive? All the apps, video, social networks, and just plain curiosity. Kvedar makes the following statement.
Many have talked about the transformational possibilities of mobile health including: the opportunity to use an always on, always connected device to message you in-the-moment about health; to capture health-related information about you via the camera and through connected sensors; and, of course, the ability to display relevant information in context. All of these are exciting, but if we can exploit the addictive quality of smartphones, it will be the most important characteristic of mobile health as we move forward.
Here are his strategies for doing the above:
1. Make it about life: Learn what the person wants from life his/her aspiration and tie health related messages to those aspirations.
2. Make it personal: Put it in the context of the phone user in relevant ways. Personalized medicine
3. Reinforce Social Connections. We all want connections to others and especially around health problems or questions we are seeking to solve. They are very powerful tools and as Kvedar notes not just for friends and family but for accountability and adherence to care and wellness plans.
Here are the tactics that are offered:
1. Subliminal Messaging. “Imagine if every time you checked your phone, an unobtrusive brief message appeared on YOUR health issue and how to improve it.”
2. Use Unpredictable Rewards. ” B.F. Skinner proved that operant conditioning is more effective when the stimulus and reward are tied only some of the time.”
3. Use Sentinel Effect. “This effect of having an authority figure look in on your life is a really powerful tool that can be used to effectively promote good health through mobility.”
Kvedar ends with reference to this in the Boston Globe
What’s going on here? We’re witnessing the death throes of advertising’s “Mad Men” era, and the birth of the Mr. Spock era. Mad Men were all about coming up with clever ideas for ads, treating clients to steak-and-martini dinners, and putting TV spots on the most popular shows. You didn’t know exactly who saw your ad when it ran on “Bonanza,” or what impact it had on sales, but you knew it reached a lot of people.
Mr. Spock is all about making logic-driven decisions based on data collected about consumers and the context surrounding the ad. Who is clicking, and is that click leading to a transaction? Is this ad worth what we’re paying?
I agree with his premiss we should leverage the smartphone we are all addicted to in order to maximize the technology that will drive outcomes and improved patient care. I agree that for this to work we need to determine what the patient wants or needs. Where I split hairs is around how we do that? Using surrogate markers of sites visited or other behaviors on the phone or even the computer is not accurate and may not directly address the problem the patient wants to solve. What needs to be done are for patients to say I need to understand this about myself and my health. I want to opt in and I want to opt in with a trusted partner or partners.
The problem here is that will we ever reach a critical mass of patients who will drive community outcomes? Will we be able to go beyond those who are active healthcare participants and move to the next demographic those who have a minor interest? This is similar to getting the young invincible’s to sign up for ACA. How can we apply all these ideas to successful marketing?
Overcoming Fragmentation in Health Care
John Noseworthy writing on the Harvard Business Review Blog Network addresses the reality that the quality of healthcare in America is fragmented which drives ‘unsustainable health care spending.’
Noseworthy points to the fact healthcare is in the throws of consolidation through mergers and acquisitions and that is at the root of fragmentation because the larger and more complex a system becomes the greater its fragmentation and cost.
It is different at the Mayo Clinic
At the foundation of our approach is a knowledge-management system — an electronic archive of Mayo Clinic-vetted knowledge containing evidence-based protocols, order sets, alerts and care process models. This system, which can be made available to physicians in any location, brings safer care, better outcomes, fewer redundancies, and ultimately cost savings for our patients. Ask Mayo Expert, one of the many tools in our system, helps physicians deliver safe, integrated, high-quality care. Through this system, physicians can find answers to clinical questions, connect with Mayo experts, search national guidelines and resources, and find relevant educational materials for patients. This knowledge is updated in real time and made widely available.
Knowledge and access to knowledge is the single most important driver of better patient care. HCP are life long learners and being able to quickly and easily access experts etc. will slow fragmentation and hopefully slow cost expansion. And that is achieved through the following activities
Through this commitment, Mayo Clinic physicians and scientists have contributed more than 400 peer-reviewed papers on quality improvement in the last five years.
Noseworthy ends with this
To transform health care in America into high-quality, patient-centered care that the nation can afford, we must address fragmentation, we must address variable quality, and we need to create a sustainable health-care financial model. Collaboration is key. Mayo Clinic has a long history of innovation focused on improving the value of health care, but we can accomplish much more by working together — integrating and sharing knowledge with one another.
This is mom and apple pie and spot on regarding learning and how it drives change. What was missing for me was the patient component. Clearly Mayo Clinic is patient centric in its care. That is known and proven but I was surprised to see it not referenced or tied to this article. Fragmentation is the the goal of the institution but the patient is at its center and can benefit if not address fragmentation. Just to make sure I didn’t miss a patient reference I searched the article and the only reference to patients was in the comments.
Great blog! First off, please let me commend you on the amazing work that you, your organization and your employees do everyday. The software you reference to address fragmentation on the hospital side sounds fantastic! May I ask how you are addressing fragmentation in the eyes of the patient? We launched a pilot program in Cleveland, OH that used Lay Patient Navigators to decrease fragmentation. By developing key relationships with patients, the lay navigators were able to massively decrease fragmentation and positively impact patient outcomes. It was a very successful program! Not only did it decrease fragmentation and increase both outcomes and patient satisfaction – it also positively contributed to the hospital’s bottom line! Just another way to think about decreasing fragmentation in the eyes of the patient because as we all know – this health care system is incredibly fragmented and confusing! Do you use lay patient navigators?
We should not forget that the patient is at the center of care and they drive our brave new world of patient engagement.
The legal justification for mandate penalty/open enrollment realignment
Nicholas Bagley a University of Michigan Assistant Professor of Law submitted a quest post to The Incidental Economist. Let me see I can explain this, the Obama administration offered guidance to ease concerns surrounding the imposition of the individual mandate using “hardship exemption”.
Here’s what the administration is worried about. Under the ACA, an individual doesn’t get slapped with the mandate penalty until she’s gone without health insurance for a full three months. That means she’s got to be covered before April 1 rolls around—which is to say, by midnight on March 31. By regulation, a plan that is purchased in the first half of a month takes effect on the first day of the following month (e.g., a plan bought on February 10 takes effect on March 1). For coverage purchased in the second half of the month, the coverage period starts on the first day of the month after that (e.g., a plan bought on February 20 takes effect on April 1). As a result, to get coverage that kicks in before April 1, an individual has to purchase a health plan by mid-February.
Yet the open-enrollment period lasts all the way through to the end of March 31.
Still, the administration is right that the awkward conjunction of the ACA and the coverage-effective dates has created a trap. Pretty much everyone who purchases insurance in the open-enrollment period will assume—reasonably if wrongly—that they’ve done what the mandate requires of them. That shared assumption provides an eminently plausible basis for invoking the hardship exemption: the assumption, by encouraging delayed enrollment, means that loads of people will face a financial penalty they hadn’t anticipated. That penalty, even if it’s assessed after the fact, will reduce their “capability” to afford the health plan that they purchased. Invoking the hardship exemption to deal with that reduction in capability makes sense, especially because the whole point of the exemption is to alleviate affordability concerns.
I have a headache trying to figure this out and understand it. Bagley has some terrific links and information which helps. But more importantly I believe the ACA is organic and will move forward in fits and starts to what I hope becomes a valid and working healthcare model. What frightens me is the fact that this looks like how sausage is made at its worse. I wonder how much faith we can hold on to while we wait for some positive metrics?
Notes & Links: October 21, 2013
Yesterdays news today. Sorry but life got in the way of life.
Just How Bad Is That Federal ACA Health Care Exchange Problem Anyway
Tim Worstall, Contributor at Forbes hits us with the good stuff. This was written prior to the speech by Obama on ACA which for now I will allow others with an ax to grind to parse its meaning. Clearly the execution of this technology has failed. And it appears from this article and from Obama’s comments a lot of code will need to be rewritten. Worstall makes a great point and one that is at the core of this issue
It’s not just Java for the script kiddies, for sure, but the complexity is actually in the design, not the programming. That design should have been nailed down two years ago, the code written and then tested for a good 6 months. Rather than what actually happened, which was that the design itself was still changeable into September of this year. That those insiders are still misdiagnosing the problem shows quite how far out of a technical understanding they are. There is this:
This is a good article in light of Obama’s speech. But it is even more important when you consider this Poll: Majority believe healthcare website problems indicate broader issue with law.
Fifty-six percent of Americans say the website problems are part of a broader problem with the law’s implementation while just 40 percent see the website problems as an isolated incident.
The bungled rollout has not soured support for the health law overall, however. Forty six percent now support it while 49 percent oppose it. That compares favorably to a 42 to 52 percent negative split last month.
Somewhere in this long painful road to healthcare in America is a Harvard Business School. I hope this ends with something more, better patient care, bending of the cost curve, improving outcomes, and just giving Americans a chance to live better
New Obamacare Numbers – Success Or Failure?
Dan Munro contributor at Forbes looks at the numbers from the state exchanges and talks about his experience applying. Today the administration said about 476,000 health insurance applications have been filed through federal and state exchanges. It remains a mystery on how many people have actually enrolled in the insurance markets. But to note a bit over half of those are from 36 states where the Federal Government is running the markets. The remaining half is from state run exchanges.
Munro ends with this and keep in mind the ACA is the single biggest target on the presidents back and when those of a certain ilk are looking to be haters ACA/Obamacare is what to aim for.
All of which suggests that rendering a success or failure verdict at this early stage (based almost entirely on the initial and poor performance of the public exchanges) seems premature. Either way, success or failure, one thing remains certain. We’re likely to see a lot more political math between now and the end of the year.
Study adds to growing recognition hat improving graduation rates can improve public health
The Pump Handle on Science Blogs has post by Kim Krisberg looking at new data showing that dropping out of high school increases the risk of illness and disability in young adulthood. Here is the open access to BMC Public Health here
Interesting to note that high school graduation was never singled out as a major public health objective. And the data clearly shows the link between morbidity and mortality.
Among the results, study authors found that the risk difference for long-term sickness or disability between those who complete high school and those who drop out was 21 percent. And even after adjusting for the accompanying risk factors listed above the risk difference was still 15 percent.
Krisberg shares some data regarding the US drop rate and the fact it has declined from 12% in 1990 to 7% percent in 2011 with rates declining among whites, black, and Hispanics. Now I guess the question becomes do we use a health strategy to drive getting a high school diploma or do we drive the message that a high school diploma will help you live longer?
Notes & Links: October 7, 2013
Why Are ObamaCare Opponents So Vehement?
David E. Williams posting on HealthWorks Collective gives us perhaps the most rational answer to the above question I have seen. Short and sweet but cuts to the chase in all this insanity of stopping ObamaCare even if we destroy our economy and the global economy.
Why they feel the way they do
- They feel the legislation was rammed down their throats and they were disenfranchised
- They honestly feel ObamaCare will be the ruination of the world’s greatest health care system
- They believe ObamaCare will bankrupt the country
- The bill is too complicated
- They want to appeal ObamaCare and replace it with something better
I buy those. Williams shows why none of those reasons hold water in a clear and on point fashion. But for me the most telling reason is the one he ends with…
A more objective read is that some opponents have whipped themselves into a lather over their revulsion to all things Obama and are living in an echo chamber where these views seem rational. It would be better for everyone if they went back to the Birther madness.
Security Concerns to Be Considered When Downloading Human Immunodeficiencey Virus/Sexually Transmitted Disease Related Smartphone Application
A letter to the editors of JMIR from Brito-Mutunayagam addresses a recent article reviewing Mobile Phone Apps for the care and prevention of HIV and other STDs. The article addressed security concerns. Brito-Mutunayagam says the bigger concern is that if an app is not developed by a a named professional health care body or organization.
It is a great letter and fits with the current trend of showing data regarding medical apps and the outcomes they deliver. Well worth the read.
A Web-Based Tool to Support Shared Decision Making for People with a Psychotic Disorder: Randomized Controlled Trial and Process Evaluation
Van der Krineke, Emerencia, et al out of the University of Groningen Leeuwarden, Netherlands published this RCT. There has been a great deal written and studied on shared decision making. Here is a good overview on the topic for some background.
Methods: The study was carried out in a Dutch mental health institution. Patients were recruited from 2 outpatient teams for patients with psychosis (N=250). Patients in the intervention condition (n=124) were provided an account to access a Web-based information and decision tool aimed to support patients in acquiring an overview of their needs and appropriate treatment options provided by their mental health care organization. Patients were given the opportunity to use the Web-based tool either on their own (at their home computer or at a computer of the service) or with the support of an assistant. Patients in the control group received care as usual (n=126). Half of the patients in the sample were patients experiencing a first episode of psychosis; the other half were patients with a chronic psychosis. Primary outcome was patient-perceived involvement in medical decision making, measured with the Combined Outcome Measure for Risk Communication and Treatment Decision-making Effectiveness (COMRADE). Process evaluation consisted of questionnaire-based surveys, open interviews, and researcher observation.
Conclusions: The development of electronic decision aids to facilitate shared medical decision making is encouraged and many people with a psychotic disorder can work with them. This holds for both first-episode patients and long-term care patients, although the latter group might need more assistance. However, results of this paper could not support the assumption that the use of electronic decision aids increases patient involvement in medical decision making. This may be because of weak implementation of the study protocol and a low response rate.
Shared decision making is important and there have been any number of reviews, analysis, and RCT here, here, and here. And here is a great site in Canada using SDM. It is simple in its concept and offers important and critical outcomes for patients. But at times it strikes me that we are making this far more complex and involved. Donna’s oncologist at our first meeting drew a horizontal line on a chart note. On the left side of the line he wrote me on the left side of the line he wrote you (Donna). He said ” Place an X how you want to work together to make decisions regarding your care. On the left I will make all decisions. On the right you make all the decisions.”
This is shared decision making succinctly presented and adhered to. This may not fit all patients but what it does do is open the discussion and create a sense of engagement and empathy which is the foundation for SDM.
Notes & Links: August 19, 2013
iPad Applications in the Healthcare Industry: Fad or Future?
Todd Riddle posting to Healthworks Collective takes a look at apps on the iPad and its utility for both patient and HCP. There has been a huge growth of iPad apps in healthcare albeit slower due to legal, medical, and patient issues. But it is changing rapidly and growing. Riddle quotes data that states by 2015 there will be 500 million smartphone users accessing healthcare application. Pretty impressive.
Advantages of iPad healthcare apps
- Patient safety
- Easy access to information
- Increases efficiency
- Minimizes costs
- Effective use of audio, video, visual communications modes
Challenges
- Not always accurate and consistent (I believe we need to expect studies on apps and outcomes
- Security and confidentiality
- Regulatory challenges
Top iPad healthcare applications
- Medscape
- MedPage Today Mobile
- AHRQ ePSS
- Radiology 2.0: One Night in the ED
- Calculate by QxMD
Riddle concludes with
Since healthcare apps are extremely sensitive, it is developer’s responsibility to rigorously test app. Quality compromises could be costly. It is equally important that user conducts a thorough due diligence of app such as checking developer’s bio, user feedback, and its reputation on the net before actually installing/using it.
Jenny McCarthy and the Selling of e-Cigarettes
Orac on ScienceBlogs points out Jenny McCarthy is now hocking blu eCigs. Now this is the same Jenny McCarthy who is anti vaccine since it is an unproven cause of autism. Let’s think about this. No evidence based proof of the link between vaccinations and autism but there are clear causative data about tobacco and disease. Orac goes into great detail to examine the data on eCigs and clearly we don’t know yet.
Although short term studies of e-cigarettes appear not to have found any evidence of significant harms, there are currently no solid long term data regarding the effects of inhaling the vapors produced by e-cigarettes. A recent review concluded that the vapors are likely safe, but did so based on primarily on a review of chemical analyses of e-cigarette vapor. A more recent analysis finds some toxic chemicals in e-cigarette vapor butat much lower levels than in tobacco smoke. Again, however, there are no long term epidemiological or observational data in actual humans using e-cigarettes.
This is an excellent review of eCigs but more important how the hell can Jenny McCarthy do this while trashing vaccinations?
What Americans Don’t Know About the Affordable Care Act
Danyell Jones posting to HealthWorks takes a look at where we as a nation stand with our knowledge of ACA and offers ways we can learn more and be better informed.
There is the chart from Kaiser Family Foundation showing that country feels we will be worse off.

